Pain
Overview
The biggest myth about pain related to cancer is that people with cancer must endure it. It is true that pain affects most people with cancer, but no one has to accept pain as a permanent part of life. There are now many ways to relieve cancer-related pain, and it’s important to understand these options and find out which option will work best for you. Although success cannot always be guaranteed, it is reasonable to expect your doctors to work diligently toward alleviating your pain.
About 90 percent of all cancer-related pain can be successfully managed, yet only half of people with pain seek relief. Why is this? Doctors have noted many reasons why patients do not seek help for pain relief:
- Guilt – they don’t want to hurt their doctor’s feelings.
- Fear – they are afraid that if they hurt, it means the treatment isn’t working or the cancer has gotten worse.
- Acceptance – they feel that pain is just a part of the cancer experience.
- Pride – they feel they should just be tough, live with the pain and not complain.
- Fear of addiction – many patients may forgo medications for fear of becoming addicted.
- Overwhelmed feeling – there are already too many doctors, appointments and medications to handle; they don’t want to add yet another aspect to their treatment plan.
You should not let any of these reasons keep you from finding pain relief. Every person with cancer is encouraged to seek relief.
Harmful effects of unrelieved pain
Unrelieved pain affects every part of your life. Your body’s disease-fighting abilities are lowered when you’re in pain, interfering with your health and recovery in general. Other side effects can also be intensified when you’re in pain, and depression often occurs when pain is unrelieved over a long time. In addition, pain affects your ability to sleep, work and maintain your relationships. These harmful effects make pain too important to ignore.
Benefits of pain relief
Pain relief has many benefits beyond the obvious one of being more comfortable. Studies show that when people with cancer get their pain under control, they are much more likely to finish their treatment on schedule. Pain relief also enables people to be more active, boosting their health and emotional well-being. Some evidence even suggests that survival is longer when pain is managed effectively.
Be your own advocate
Every doctor wants the best for his or her patients, but it is impossible for every doctor to know about all of the ever-expanding options for pain management. That’s why a pain specialist plays an important role in the care and treatment of people with cancer-related pain. If your pain is unrelieved, tell your doctor that you want to see a pain specialist. With a physician who has expertise in pain management on your treatment team, your comfort will be a top priority throughout your treatment and recovery.
It may also be helpful to reach out to other people with cancer to learn about pain relief options that worked for them. Although each person responds differently to pain relief treatment, those who have found a successful approach can be a valuable resource for you.
Know your options
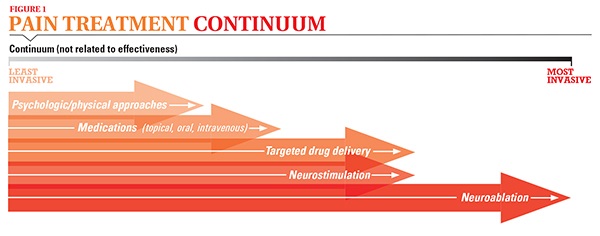
Most people think that the only way to relieve pain is to take medication. But there are many ways to manage pain, and they run on a continuum from least to most invasive (see Figure 1). You may not necessarily advance through the continuum on a straight line; depending on the particular situation, a more invasive procedure may be given before a less invasive one. Your doctor will discuss the various options and choose an order of options that seems best. Some psychologic/physical approaches may help alleviate mild pain, and these approaches are often valuable when used in combination with other treatments for more severe pain. Pain medications are the next step on the continuum. In this content, you can learn about the wide range of pain medications now available and how they’re used. You will also learn about interventional approaches that are options when medications fail to relieve pain. These interventions include targeted drug delivery; nerve blocks; percutaneous procedures on the spine; neurostimulation; neuroablation; and palliative radiation, chemotherapy and surgery. These interventions can be used in combination with lower doses of pain medication if necessary.
This content also provides information on integrative oncology approaches, or evidence-based complementary therapies that can be used in conjunction with other pain management techniques. You will also learn how rehabilitation cancer care, which focuses on restoring function and movement, can help in managing pain. Lastly, you will learn about the emotional aspects of pain and how to address these issues.
Be sure to review the resources here to find help on your path to pain relief. Do not let pain control your life — control your pain and take back your life.
Myth vs. Fact - cancer pain and its treatment
Myth: Increasing pain means that my disease is getting worse.
Fact: Pain and severity of disease are not necessarily related, but increasing pain should prompt a conversation with your doctor evaluate the cause and develop a plan for more acceptable pain relief.
Myth: I don’t want to have unpleasant side effects from pain medications.
Fact: Side effects may occur with some pain medications, but they can be managed and some will decrease or disappear over time on their own. If you become tolerant to your medications or the side effects are too difficult, a health care provider with expertise in cancer pain can help guide you through other options.
Myth: If I take narcotics (opioids) regularly, I may become addicted.
Fact: Although people can become tolerant to a pain medication (meaning more doses are required to have the same effect), tolerance is not the same as addiction. Addiction is a specific diagnosis in which people act in risky or abnormal ways to get drugs. People with cancer who take pain medications as directed usually don’t become addicted.
Myth: If I start taking pain medication early on, I will run out of options for pain relief in the future.
Fact: Many pain-relieving medications and procedures are available. More options are available if pain becomes more severe.



