Advanced Prostate Cancer
Radiation therapy
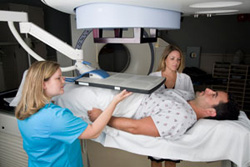
This type of therapy uses high-energy radiation to kill cancerous cells and shrink tumors.
Adding ADT to radiation treatment improves survival in men with locally advanced prostate cancer. Radiation therapy is more commonly used for earlier-stage prostate cancer but is an option for locally advanced prostate cancer as well. Radiation is also effective in reducing pain or shrinking tumor masses pressing on organs or the spinal cord among men with cancer that has progressed to the bones or other organs.
Radiation therapy options
- External-beam radiation therapy (EBRT) comes from a large machine outside the body that aims high-energy X-rays at the cancer site. Treatments are usually given five days a week and may last eight to nine weeks. EBRT may be used alone or in combination with brachytherapy (radioactive seed implants) for locally advanced prostate cancer. Intensity-modulated radiotherapy (IMRT) or image-guided radiotherapy (IGRT) as well as proton beam radiation are also used for locally advanced cancer. In addition, EBRT or IMRT may be used to treat specific sites of cancer that have spread to the bones to reduce pain or prevent fractures.
- Radiopharmaceuticals are given intravenously and include a radioactive substance that gives off low levels of radiation. Ideally, this radiation travels primarily to the cancer deposits in the body.
Radium-223 is used in men with metastatic, castration-resistant prostate cancer that has spread to bone but not to other organs. Radium-223 is processed in the body like calcium and deposited in areas of bone damaged by cancer. There it delivers radiation to cancer cells but has a limited effect on normal surrounding tissues. Treatment is usually given every four weeks for a total of six doses. Studies have shown that, compared with standard supportive therapy (prednisone), radium-223 improved survival and lengthened the time to a bone complication (such as a fracture or spinal cord compression) or the need for radiation to treat bone-related symptoms.
Strontium-89 and samarium-153 are two other radiopharmaceuticals that are effective in relieving metastatic bone pain, but unlike radium-223, they have not been shown to improve survival. They also have a high risk of bone marrow suppression, which means your marrow has a decreased ability to produce blood cells. Bone marrow suppression may limit your options for other treatments.
Side effects
Radiation therapy may cause the following side effects, especially in the later weeks of treatment:
- Fatigue
- Frequent urination or burning with urination
- Dry, red and tender areas at radiation site
- Inflammation of the lining of the bladder, rectum or small intestine, resulting in urinary and bowel problems, such as frequent urination and incontinence (inability to hold urine or bowels). Loss of erection may also occur in the later stages of treatment.
Common side effects of radiopharmaceuticals include nausea, diarrhea, vomiting and swelling of the legs and feet.
Monitoring response
After radiation therapy, your PSA level should be checked every six months, and you should also undergo a physical examination (including a DRE). Imaging tests will be done if the PSA level begins to rise. Tell your doctor about any concerns you have or new symptoms you experience after treatment.
Questions about radiation therapy you may want to ask your doctor
- Which type of radiation is an option for me?
- How often will I have treatments? How long will they last?
- How will I feel during the treatments?
- How will I feel when the treatments are done?
- Will my activities be limited?
- Will I need to stay in the hospital?
- What are the side effects? Are there any long lasting effects?
- What is the chance that the cancer will come back?
- How often will I need checkups once treatment is over?
- How will radiation therapy affect my sexual well-being and fertility?
- What are the costs of radiation therapy and will insurance cover it?
- Is there a clinical trial that I may be eligible for?



