Follicular Lymphoma
Staging
Staging is how physicians determine the extent of cancer. Staging of hematologic (blood) cancers, such as lymphoma, differs from staging for most other cancer types. For example, solid tumors are typically staged based on the size of the tumor, whether regional lymph nodes contain cancer and whether the cancer has spread beyond the original site. Hematologic cancers are often classified or staged according to other factors, such as the type and subtype, the microscopic appearance of the lymphoma cells, lab results, chromosome abnormalities or the results of molecular testing, in addition to the specific sites of involvement. Different classification systems are then used to describe these factors as they relate to your diagnosis.
The Lugano Classification System* is the most commonly used system for staging non-Hodgkin lymphoma. With this system, lymphoma is assigned a stage of I, II, III, or IV, with or without additional factors. These stages can be divided into two groups: limited stage and advanced stage.
Table 1. Lugano Classification for Hodgkin and Non-Hodgkin Lymphoma
| Stage | Description |
| Limited Stage | |
| Stage I | Involvement of a single lymphatic site (i.e., nodal region, Waldeyer’s ring, thymus or spleen). |
| Stage IE | Single extralymphatic* site in the absence of nodal involvement (rare in Hodgkin lymphoma). |
| Stage II | Involvement of two or more lymph node regions on the same side of the diaphragm. |
| Stage IIE | Contiguous (touching or near) extralymphatic* extension from a nodal site with or without involvement of other lymph node regions on the same side of the diaphragm. |
| Stage II bulky** | Stage II with disease bulk. (Bulk is defined as a mass greater than one third of the thoracic diameter on CT of the chest or a mass more than 10 cm.) |
| Advanced Stage | |
| Stage III | Involvement of lymph node regions on both sides of the diaphragm; nodes above the diaphragm with spleen involvement. |
| Stage IV | Diffuse or disseminated involvement of one or more extralymphatic* organs, with or without associated lymph node involvement; or noncontiguous (not touching or near) extralymphatic organ involvement in conjunction with nodal Stage II disease or any extralymphatic organ involvement in nodal Stage III disease. Stage IV includes any involvement of the CSF (cerebrospinal fluid), bone marrow, liver or multiple lung lesions (other than by direct extension in Stage IIE disease). |
In addition to this staging system, some oncologists may also use the Follicular Lymphoma International Prognostic Index (FLIPI) to predict the risk of disease recurrence and overall survival. The FLIPI, which may also be referred to as FLIPI-1, takes into account the age and general health of the patient, the stage of the disease, the level of hemoglobin (a substance that carries oxygen throughout the blood), the number of involved lymph nodes, and the presence or absence of elevated levels of an enzyme called lactate dehydrogenase (LDH) in the blood.
The FLIPI assigns one point for each of the following risk factors:
- Age older than 60 years
- Late-stage disease (Stage III or IV)
- Hemoglobin level less than 12 g/dL
- More than four involved lymph node areas
- High LDH level
The overall FLIPI score is the total number of points assigned to a patient. The lower the score, the better the prognosis (predicted outcome from treatment).
Lastly, the World Health Organization recommends that follicular lymphoma be assigned a histologic grade, which is determined by the appearance of cells under a microscope. The grade defines how aggressive the cancer cells are likely to be and helps doctors make various treatment decisions, including when treatment should start. The higher the grade, the more likely the disease is to progress.
Table 2. Histologic Grades of Follicular Lymphoma
| Grade | Definition | ||
| 1 | 0-5 centroblasts per high-power field | ||
| 2 | 6-15 centroblasts per high-power field | ||
| 3 | More than 15 centroblasts per high-power field | ||
| 3A | Centrocytes (smaller cells) still present | ||
| 3B | Solid sheets of centroblasts | ||
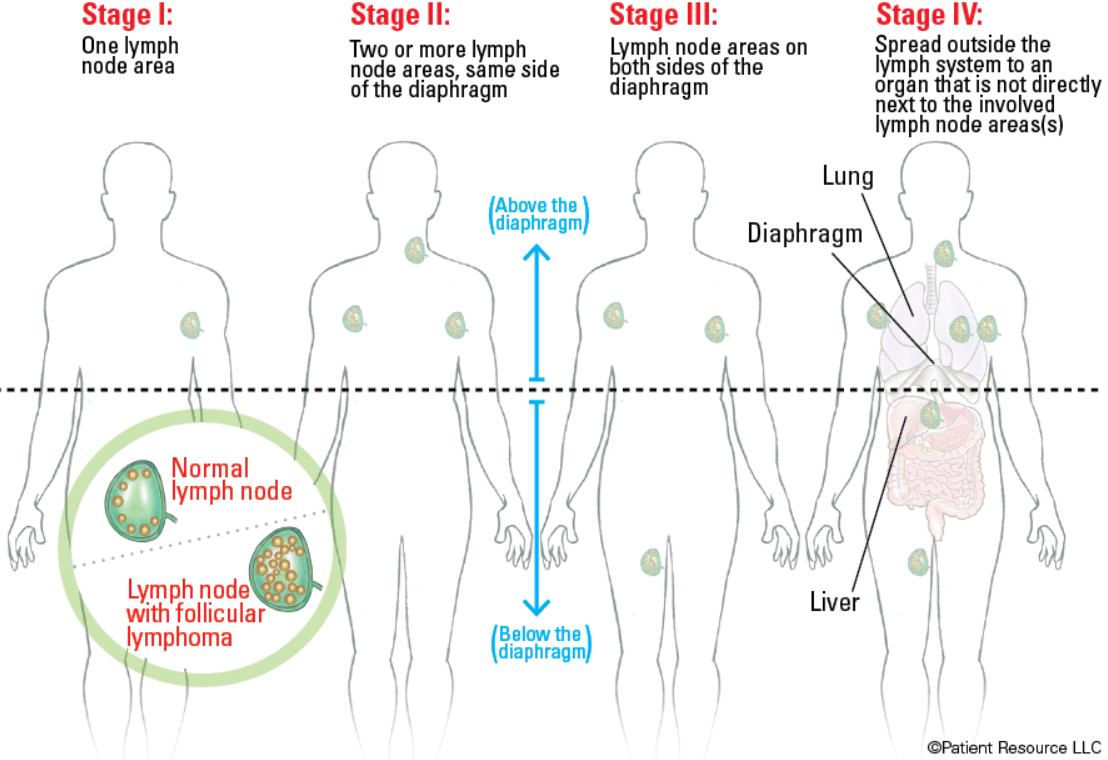
Stages of Follicular Lymphoma
Follicular lymphoma is staged according to how many lymph nodes are affected and where they are in the body. The dotted line below indicates on which side of the diaphragm the affected lymph nodes are.