Lung Cancer
Introduction
You may have just been diagnosed with lung cancer, but you can take comfort in knowing that medical professionals, scientists, researchers, health care workers, support groups, survivors and anyone who has been touched by lung cancer are members of a tight-knit community. In their own way, each contributes to the significant advances that are being made in treating and managing the disease. From developing groundbreaking therapies to sharing valuable advice, together they, and now you as well, are working toward the shared goal of curing lung cancer.
Lung Basics
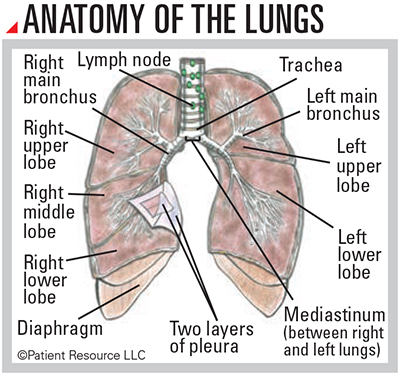
Your lungs are a pair of large, spongy, expandable organs in your chest cavity. The right lung is a little larger and has three parts (lobes); the left lung has two. They are surrounded by a thin layer of protective tissue (pleura).
When you inhale, your lungs absorb oxygen, which is delivered to neighboring red blood cells that then carry the oxygen to the rest of your body. When you exhale, your lungs rid the body of carbon dioxide. Your diaphragm helps your lungs expand and contract when you breathe.
Cancer develops when abnormal cells in the lining of the airways accumulate to form a tissue mass. This is called a primary tumor. It may grow into the lining around the lung and form secondary tumors nearby. People with lung cancer often have chronic pulmonary disease in the non-cancer tissues of the lung, which may interfere with lung function and change treatment options. Pulmonologists often assist
in assessing lung function and work closely with oncologists (see Get to Know Your Health Care Team).
When lung cancer cells break away and enter the bloodstream to form tumors in distant sites such as the opposite lung, liver, brain or bones, the disease becomes advanced. These tumors are known as metastases. Although they are in other parts of the body, they are still considered lung cancer and are treated as such.
Types of Lung Cancer
Lung cancer has two main pathologic types: non-small cell lung cancer (NSCLC) or small cell lung cancer (SCLC). This guide focuses on NSCLC, the more common of the two.
NSCLC has several subtypes:
- Adenocarcinoma is the most common NSCLC subtype, especially in people who have never smoked. It usually grows more slowly than other types and tends to spread to distant sites more often than other types, except for SCLC.
- Squamous cell lung cancer (epidermoid carcinoma) is the second most common subtype. It spreads to distant sites less often than adenocarcinoma.
- Large cell lung cancer is the least common type of NSCLC. It tends to grow and spread quickly. When large cell lung cancer includes neuroendocrine features, such as higher-than-normal amounts of hormones, it may behave and be treated like SCLC. Other times it may have features more like adenocarcinoma.
SCLC is named for its appearance under a microscope. It is an aggressive form of lung cancer and most often spreads to distant parts of the body before it is found. Research is underway to explore SCLC subtypes and how they may respond to treatment.
Less common types of lung cancer include mesothelioma, typical and atypical carcinoid tumors and sarcoma. These and others can begin in other organs.
Seeking a Second Opinion
Even though you may trust your doctor completely, you deserve to gather as much information
as possible about your diagnosis and treatment options. Seek a second (or third or fourth) opinion of a lung cancer specialist; if possible, find a physician who has experience treating a diagnosis similar to yours. The additional input will confirm your pathology report, diagnosis and stage, and you will benefit from the unique training and experience each doctor brings.
You may be concerned that you will offend your doctor. Most doctors welcome a second
opinion and are often pleased to give you a referral. The ultimate goal is for you to get the best care possible.
You may also feel you have to begin treatment right away. Generally, unless your diagnosis is extremely advanced, you can take the time to explore your options and make the decision that is right for you.



