Radiation Therapy
Planning Your Treatment
Before you begin radiation therapy, you will meet with a radiation oncologist to determine whether radiation is appropriate for you. The doctor will review your medical history and may perform a physical exam. You will likely discuss the potential benefits and risks of radiation therapy, and you’ll have the opportunity to ask questions. Once you’ve decided to include radiation as part of your treatment plan, you’ll be asked to sign a consent form.
Informed consent
A radiation treatment consent form gives the doctor permission to treat you with radiation and complete the necessary testing for treatment planning. Although the details of the consent form may vary, it generally states that your doctor has explained the potential benefit of radiation therapy for your diagnosis, as well as the possible risks, the type you’ll be receiving and any other treatment options you may have. By signing the form, you confirm that you’ve received and understood this information and that you agree to treatment with radiation and are aware that treatment does not guarantee the intended results.
Your radiation team
Your radiation treatment team will include several professionals trained in radiation therapy:
- Radiation oncologist – treats cancer with radiation and is in charge of managing your radiation treatment plan and working with other treatment team members.
- Radiation oncology nurse – cares for patients receiving radiation treatment and is available to answer your questions about radiation and tell you how to monitor your health and manage or prevent possible side effects.
- Radiation physicist – makes sure the radiation equipment works properly, including delivering the correct dose of radiation as prescribed by your radiation oncologist. The radiation physicist also helps develop the treatment plan.
- Radiation dosimetrist – works with the radiation oncologist to plan treatment and calculate the appropriate radiation dose.
- Radiation therapist – delivers the radiation, typically daily, during scheduled treatments, ensures that you are positioned properly for each treatment and operates the radiation equipment.
Your team may also include additional health care professionals, such as a dietitian, physical therapist or social worker, as needed.
Simulation
The first radiation therapy session will be a simulation to help with the planning. During the simulation, your treatment team will use imaging scans to determine exactly where the radiation beams need to be directed. This may include the following imaging techniques:
- Computed tomography (CT) – CT is a procedure in which a scanner creates three-dimensional X-ray images of the organs, tissues and bones inside the body and displays cross-sectional pictures of them on a computer screen. CT may also be called a CAT scan. This is the most common imaging for breast cancer treatment.
- Magnetic resonance imaging (MRI) – MRI involves the use of magnetic fields instead of X-rays to create images of structures inside the body.
- Positron emission tomography (PET) – A PET scan involves the use of radioactive substances (tracers) that travel through the blood stream and collect in areas of fast metabolism (cells that use a lot of energy), such as tumors. The machine then detects those areas and creates images that help the doctor determine where the cancer cells are located. Often, PET may be combined with CT, which is known as a PET/CT scan.
- Ultrasound – Ultrasound uses sound waves to produce images of the organs inside the body and can show where the tumor is located.
Once the treatment team has determined the appropriate position for you on the table, you must be placed in exactly the same position for each treatment session. To make sure this happens, body molds or other immobilizing devices may be necessary. If you are to receive radiation to the head and neck, a special mesh head mask, called a thermoplastic mask, may be created from a mold of your face and head (see Figure 1). In most cases, semi-permanent marks or permanent tattoos may be placed on your skin to indicate the exact location the radiation beams must hit to reach the tumor.
Your treatment team will want to make you as comfortable as possible, so be sure to talk to them about any anxiety you feel, especially regarding immobilizing devices. They will work with you to find a position you are comfortable with that can be reproduced for each treatment. If necessary, your doctor may prescribe medication to ease anxiety and help you relax for your treatments.
Figure 1.
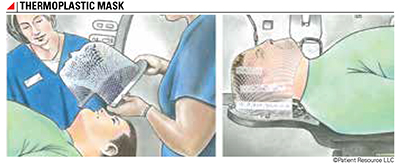
Your treatment plan
After the simulation is complete, your treatment team will calculate the appropriate dose and finish treatment planning. Different doses of radiation are used to kill different types of cancer cells. The overall dose of radiation necessary to treat your cancer is determined by several factors, including the type of cancer you have, the location of the tumor(s), the goal of treatment and your overall health. To minimize damage to normal tissue and to increase the likelihood that the radiation will kill the most cancer cells, the total dose of radiation is typically divided into several smaller doses and given over a period of time. Researchers continue to study the effects of different dosing schedules in hopes of finding more effective and convenient options for patients. For example, recent research has shown that for most patients treated with a lumpectomy, a shorter course of treatment lasting 3 to 4 weeks rather than 6 weeks is just as safe and effective.
Family Planning
Radiation therapy can affect fertility, especially if the radiation will target the pituitary gland in the brain or your reproductive organs, including the abdomen, pelvis, lower spine, ovaries or uterus. If you are receiving radiation to an area that could result in infertility but are not ready to rule out the possibility of becoming a parent, consult with a fertility expert (known as a reproductive endocrinologist). There are ways to preserve your fertility and your doctors, oncologists and fertility experts can all help you better understand your options.



