Lymphedema
Lymphedema is an excess of lymph fluid in body tissues that causes abnormal swelling of a part of the body. It is most common in an arm or leg but can occur in the neck, face, mouth, abdomen, groin and other parts of the body. General swelling can also occur, depending on the type of disease and treatment. The swelling ranges from a mild increase to extreme swelling that interferes with motion or function of the affected area (see Figure 1).
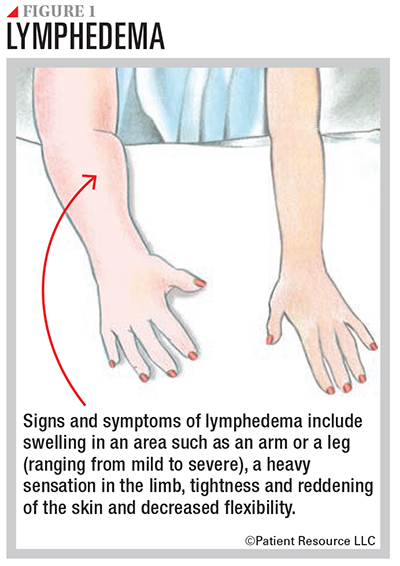
The signs of lymphedema include the following:
- Swelling in the breast, chest, shoulder, arm, hand, leg or foot
- An extremity or affected area that feels full or heavy
- Changes in how the skin in an area looks (red) or feels (tight and hard)
- New aching or discomfort in an area
- Less movement or flexibility in nearby joints (shoulder, hand, wrist, hip or knee)
- Difficulty fitting your arm into a jacket or shirt, or tightness of jewelry on your hand or wrist
What causes lymphedema?
Lymphedema occurs when lymph cannot flow normally through lymph vessels because of damage to lymph nodes or lymph vessels or removal of lymph nodes. It is typically caused by surgery to remove lymph nodes, radiation therapy that affects the lymph nodes and lymph vessels, or a blockage of the lymph nodes or vessels caused by cancer. Treatment of lymphedema is determined by the stage and severity of the condition.
Treatment of lymphedema is determined by the stage and severity of the condition.
Stage 0: The lymphatic system may have been damaged but swelling may not be visible yet. People may feel a heaviness or aching in the affected body part.
Stage I: Swelling is now visible but there are no signs of skin thickening or scarring. It can be reduced by keeping the affected limb raised and using compression.
Stage II: Skin may or may not indent when pressed. Moderate to severe skin thickening is present. Compression and keeping the limb raised may help but will not reduce swelling.
Stage III: The skin is now very thick and hardened. The limb is swollen in size and volume, and the skin has changed texture. This stage is permanent.
When does lymphedema typically occur?
Lymphedema can develop from weeks to many years after treatment begins.
How you can manage lymphedema.
The following may help minimize swelling and control discomfort:
- Avoid constriction of the area by only wearing loose clothes and loose jewelry on the affected side, carrying a handbag or backpack on the unaffected side, keeping legs uncrossed while seated and avoiding socks or stockings with tight bands.
- If you have lymphedema of an arm, avoid having injections (blood draws or vaccines) and blood pressure measurements in that arm.
- Keep blood from pooling in the affected limb by elevating it to a point higher than the heart. Do not swing the limb quickly in circles or let the limb hang down. Do not apply heat to the limb.
- Preventing infection is important because infection causes your body to respond by making more lymph, and if the lymph nodes and/or vessels are damaged, the excess fluid has nowhere to go. Keep your skin and nails clean and well-maintained.
- To decrease your risk of developing lymphedema after treatment, it is important to regain full range of motion by using exercises suggested by your health care provider.
When to call your health care provider.
Contact a member of your health care team immediately if the affected limb or body area feels hot, looks red or swells suddenly, or if you have a fever (oral temperature of 100.4°F or higher) that is not related to a cold or flu.
Report symptoms that persist for 1 to 2 weeks so treatment can begin promptly. If left untreated, it can cause more swelling, weakness or difficulty moving your arm or leg. You may also develop itchy, red, warm skin, wounds that do not heal, an increased risk of skin infections causing pain, and thickening or hardening of the skin.
A certified lymphedema therapist (CLT) may develop a treatment plan that may include complete decongestive therapy (CDT), which is a combination of skin care, manual lymphatic drainage, exercise and compression; compression garments to put pressure on affected areas, elevation and exercise; manual lymphatic drainage (MLD), which is a special type of gentle skin massage; medications for infection or pain; physical therapy; or skin care to keep the area clean and moisturized. In some cases, transplanting failed lymph nodes with healthy ones to reverse lymphedema may be an option.



